Ocular migraines are migraines that cause visual disturbances, and may or may not be accompanied by pain. The symptoms can be very frightening, and can include temporary vision loss, but your vision will return to normal.
Ocular migraine symptoms can last anywhere from five minutes to half an hour. even though you experience the symptoms of an ocular migraine, you should see your ophthalmologist to rule out other conditions which may threaten your vision.
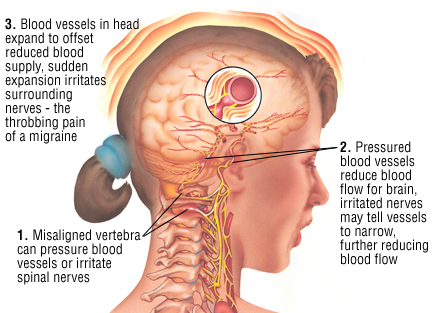
How Ocular Migraine Headaches Work
Migraines occur when a blood vessel in the brain spasms. An ocular migraine occurs when that spasm affects the blood flow, and therefore oxygen flow, to the visual processing center in the brain. Headaches may occur before, during, or after ocular migraines, or not at all.
Ocular Migraine Headache Visual Symptoms
Visual symptoms may appear in one or both eyes.
Symptoms of ocular migraines typically last anywhere from five to thirty minutes. Visual disturbances you may experience during an ocular migraine include:
Zigzagging lines of light
Shimmering light
Bright spot or streak of light
Flashing lights
Generalized bright light
Colored lights
A spot or spots in your vision
Tunnel vision
Blind spot
Loss of peripheral vision
Blurred central vision
Total loss of vision
Ocular Migraine Headache Physical Symptoms
Some people experience physical symptoms in addition to visual disturbances. Often these symptoms come after the visual disturbances. They can include:
Nausea
Vomiting
Fatigue
Dizziness
Confusion
Numbness
Ocular Migraine Headache Triggers
Nitrates and nitrites – found in processed meats, some wines, and some drinking water
Monosodium glutamate (MSG)
Fluorescent lighting, including the popular compact fluorescent bulbs
Bright sunlight
Strong odors
Excessive heat
Dehydration
Stress
Hormonal changes
Birth control drugs
Changes in barometric pressure
What to Do if You Have Ocular Migraine Headache Symptoms
Ocular migraines will not permanently rob you of your vision, but they can be dangerous if they happen during situations like driving. The symptoms of ocular migraines can be very similar to the symptoms of other problems, including retinal tear or retinal detachment. They can also mimic the signs of stroke. even though you have never had a migraine or ocular migraine before, you should talk to your ophthalmologist or see a doctor right away to rule out something more serious.
Treatment is primarily prevention. Learning your personal triggers and avoiding them is the best way to stop ocular migraines. Medications are sometimes prescribed for migraines, but they are rarely effective. Many people have successfully beaten migraines with a combination of biofeedback and avoiding their triggers.
What is Fioricet?
Fioricet is a combination medication. That is, it contains several different medications that work together to have a stronger effect.
The active ingredients in Fioricet are:
-
- Acetaminophen (the main ingredient in Tylenol)
- Caffeine
- Butalbital
Acetaminophen is a pain reliever. It starts working in less than an hour to reduce headache pain. Caffeine is also useful for fighting a headache, and it increases the effectiveness of acetaminophen. Butalbital is a barbiturate, which is a sedating or relaxing type of medication. The butalbital in Fioricet helps reduce anxiety and cuts down on the restlessness caused by the caffeine.

Hikma Pharmaceuticals USA Inc.
Pill Identification: West-ward 787
Is it effective for migraines?
Sometimes. There is very little scientific research to show Fioricet can stop a migraine. It is intended to be used for tension-type (muscle tension) headaches, which are different from migraines.
There is good research to show acetaminophen is effective at stopping migraines. Unfortunately, the dose of acetaminophen that works best to stop a migraine is lower than the dose in Fioricet.
- Fioricet can be habit-forming: Over time, your body can stop responding to a regular dose of Fioricet, which might push you to take a higher dose than you normally would. It is also possible to develop a dependency on Fioricet. In other words, you might begin to think you can’t feel normal without it. This might cause you to take Fioricet too frequently.
- Too much Fioricet can make you dangerously sleepy: Butalbital is a relaxant, and it can be harmful when combined with other relaxants, including alcohol. In large doses this effect can be life-threatening. Additionally, because Fioricet contains acetaminophen and caffeine, you should not take it with Tylenol, cold medicines that contain acetaminophen, caffeine pills, or caffeine-containing beverages like coffee, soda, or energy drinks. Both acetaminophen and caffeine are also dangerous at high doses.
- Stopping Fioricet quickly can cause withdrawal: If you’ve been taking Fioricet for a while, you could experience symptoms of withdrawal, including seizures, if you stop taking it suddenly. Talk to your provider about finding a way to lower your dose safely if this is a problem for you.
- Taking Fioricet can increase your risk of headaches: Taking Fioricet frequently can cause a different sort of headache, called a medication-overuse headache. Also, when the caffeine in Fioricet wears off, some people get a rebound headache.
- Too much Fioricet can damage your liver: The acetaminophen ingredient in Fioricet can cause damage to your liver if you take it too often. If you already have liver problems you should avoid Fioricet.
- Fioricet is not a good choice for pregnant or nursing women: If you take Fioricet while you are pregnant, your newborn baby could experience withdrawal symptoms after they are born. Acetaminophen and caffeine carry their own risks during pregnancy. In addition, all three ingredients can be passed through the breastmilk to infants who are nursing. Fortunately, there are other medications you can take if you are pregnant or nursing and need treatment for your migraines.
When should you take Fioricet for migraine?
Fioricet is best when it is used for tension-type headaches, which are different from migraines.
Tension-type headaches, which are also known as muscle contraction headaches, usually feel like a steady tightness on both sides of the head. They don’t cause nausea or vomiting and don’t get worse with movement. Unlike migraines, tension-type headaches also don’t usually get worse with bright lights or loud sounds.
For migraines, safer and more effective medications are available (see next section). If nothing else works for you, Fioricet can be a back-up option.
Regardless of why you are taking it, Fioricet should only be used occasionally.
A number of other medications are available for treating migraines. These include over-the-counter and prescription options.
-
- Over-the-counter medications
- Acetaminophen (Tylenol)
- Ibuprofen (Motrin or Advil)
- Naproxen (Aleve)
- Acetaminophen, aspirin, caffeine (Excedrin Migraine)
- Prescription medications
- Triptans, such as rizatriptan (Maxalt), sumatriptan (Imitrex), and zolmitriptan (Zomig)
- Gepants, such as ubrogepant (Ubrelvy) or rimegepant (Nurtec)
- Lasmiditan (Reyvow)
In addition, a variety of daily medications, such as amitriptyline (Amitril, Elavil), propranolol (Inderal LA), and topiramate (Topamax) are available to keep migraines from happening in the first place. Fioricet should never be used as a daily medication.
How long after taking Fioricet can you take Excedrin Migraine and other medications?
After taking Fioricet, wait at least 4 hours before taking anything else that contains caffeine or acetaminophen so you don’t overdose on these ingredients. This includes Excedrin Migraine, Excedrin Extra Strength, Excedrin Tension Headache, and Excedrin PM Headache.
Butalbital stays in your body for about 35 hours after a single dose of Fioricet. It causes sleepiness, and taking more doses of Fioricet in this time will make the sleepiness worse. Avoid alcohol or other relaxant medications while there is still butalbital in your body.
